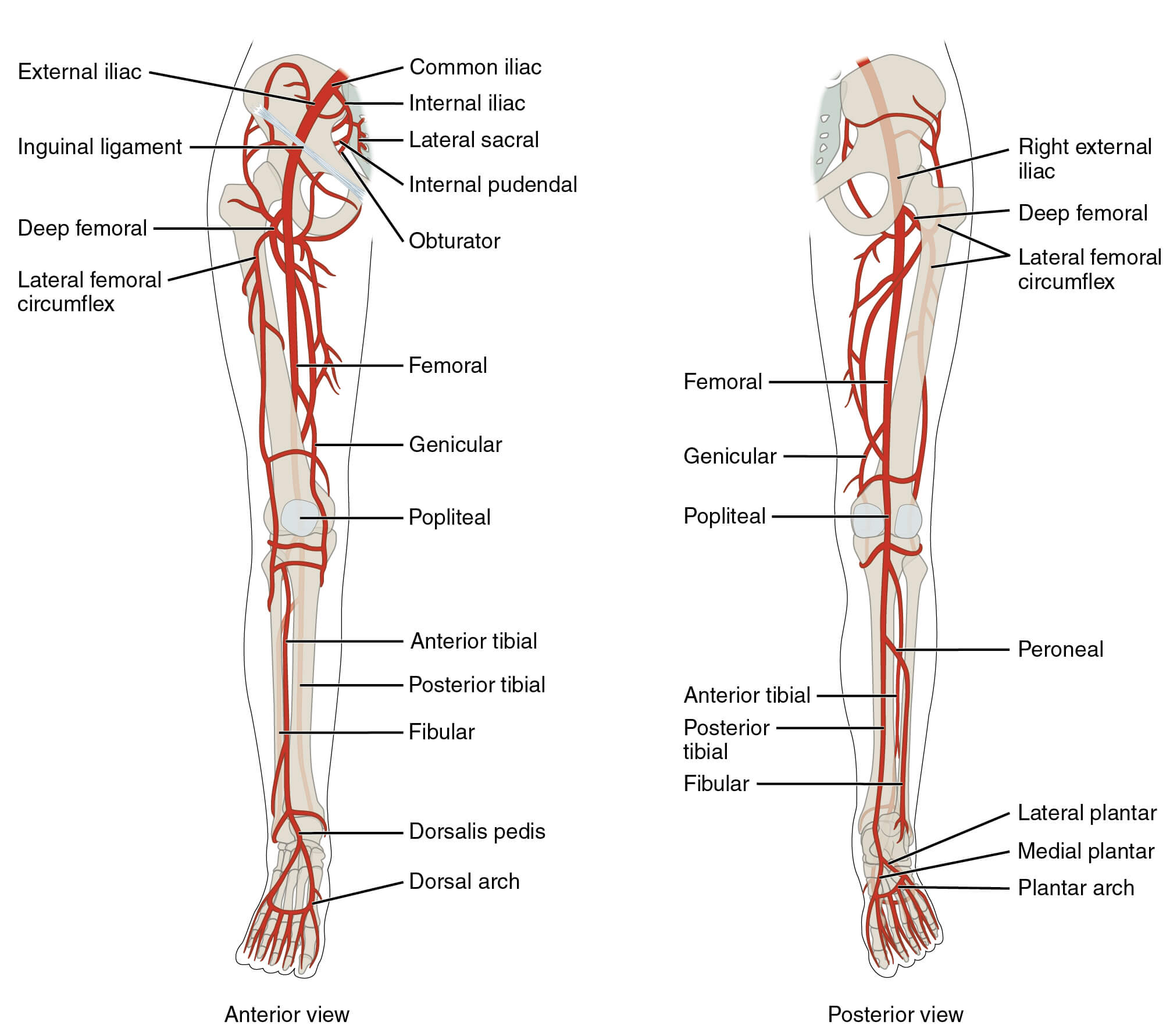
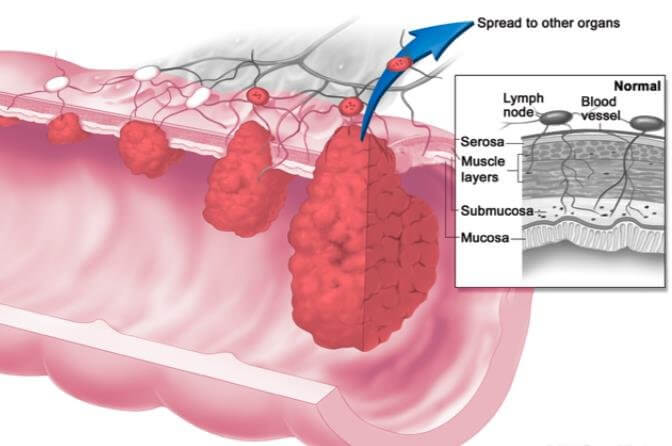
- 5 Vertebrae
- discs sandwiched between bodies act as shock absorbers
- alignment is straight.
- by definition if there is a curve 10° or more, then it is called scoliosis. < 10° is not a scoliosis.
- lordosis of the lumbar spine is due to the shape of the discs and due to the vertebrae because discs are trapezoidal.
- Anterior coloumn i.e. vertebral body + disc + ALL + PLL carry 70% of body weight.
- Facets carry 30% of body weight.
- Discs absorb shock and allow motion but have poor resistance to shear forces. So disc is fine with compression, fearful of rotation but very poor at shear forces.
- Facets resist the shear forces.
- Sacrum has a 45° angle, therefore the lower 2 discs have the greatest shear forces and therefore greatest strain on the facets.
SIJ
- SIJ has diarthrodial and fibrous portions.
- diarthrodial has hyaline cartilage + capsule + synovium + synovial fluid.
- Fibrous portion is similar to pubic symphysis.
- SIJ is a rare pain generator
Posterior Elements
- Facets – facets are restraints to motion.
- Angles of facets vary between male and female.
- Females have more sagitally oriented facets i.e they are more front to back whereas in males they are more coronal i.e. side to side.
- More sagitally oriented facets have less ability to resist shear.
- There is more shear resistance in a male facet than a female facet. This is so because females are designed to deliver children, so the pelvis has to open more and therefore there is less resistance to that.
- Spinous processes are flexion restraints through inter and supraspinous ligaments.
- Spinous processes are extension blockers because they abut each other in extension.
- Pedicles connect the anterior and posterior coloumns.
Normal Sagittal Alignment
- Lumbar lordosis: 40-60°.
- Sacral angle: 45°. Therefore L5-S1 disc is at 45° slope.
- Thoracic kyphosis: 20-40°
- Cervical lordosis: 30-40°
- Centre of C7 should be right over sacral ala.
- All curves should balance each other.
- Asymmetrical disc shapes are responsible for lumbar, thoracic and cervical curves.
Biomechanics of Spine
- Facets are connected to the spine through pedicles.
- Superior facets are embedded into the pedicles.
- Inferior facets are connected by a thin bony bridge called the pars interarticularis to the pedicles.
- facets prevent shear forces to the disc.
Ligaments
- ALL tightens with extension.
- PLL tightens with flexion
Centre of rotation is in the posterior 1/3 of the disc, so with extension ALL stretches, anterior disc stretches and posterior disc compresses.
- PLL has more stretching capacity than posterior annulus. Therefore PLL cannot protect the posterior annulus when one bends forwards. So one can tear the posterior annulus with an intact PLL.
- Ligamentum Flavum – is a flexion restraint. It is called a yellow ligament because it looks yellow. It has high concentration of a special protein called elastin. So it can stretch to good length and return to normal.
Normal Spinal Foramen
- More than 1/2 of the height of the foramen is made up by intact disc.
- Therefore with disc narrowing, one starts to lose foraminal height.
- Combined with a bone spur, it causes further narrowing. How does this happen? Reduced disc height puts too much pressure on the facet which then develops bone spur and foraminal narrowing ensues which is called foraminal stenosis.
Values of Motion
| Disc | Flexion | Lateral Bending | Rotation |
| L1-2 | 13 | 7 | 2 |
| L2-317 | 15 | 6 | 3 |
| L3-4 | 16 | 8 | 3 |
| L4-5 | 17 | 6 | 2 |
| L5-S1 | 20 | 3 | 5 |
- Average total lordosis is 40-60°.
- Average full ROM 80°.
- Highest rotation is at L5-S1 level, so this disc wears out the fastest.
Disc Height / Thickness
- Disc height increases by 0.5 to 1.00 mm at each level in lumbar spine.
- Maximum disc height is at L4-5 (up to 16mm)
- L5-S1 although has maximum ROM but is one of the thinnest in the lumbar spine. Normally L1-2 is a little thinner but L5-S1 is no more than 12 mm most of the time.
Anterior Core Muscles
Anterior muscles (rectus abdominis, transversalis, external and internal obliques) attach superiorly from the ribs to the front of the pelvis. Laterally these muscles do not attach into the vertebrae but into a retinacular sheath that then attaches to the spinous processes.
This means anterior muscles cannot directly affect the position of the vertebra. They cause generalised motion. When contracted they cause torso flexion, lateral bending and rotation and also abdominal content compression.
Posterior Muscular Contractions
- The lumbar extensors (QL & Erector Spinae) attach from the sacrum and pelvis to the thoracic spine.
- There are some small attachments to the lumbar spine but the attachments generally start at the vertebra and ascent, not descend.
- There are no muscles which insert from the pelvis to the vertebra, except for the QL and some multifidi.
Spinal Movements
There are 6 degrees of freedom.
There are no strong direct muscle attachments for 3 of the 6 directions the spine can move.
Because the spine can bend, extend, laterally flex and rotate, the muscles that control the spine have significantly more work and coordination efforts than any other region of the body. e.g. elbow only bends and extends. This is possible due to reciprocal innervation. Biceps contracts, triceps relaxes in flexion and the elbow bends. But in spine, the coordination is far too complex. We do not have this reciprocal inhibition in the lumbar spine.
Multifidus
- They are more like stabilisers, not prime movers.
- Their action is extension of lumbar vertebra.
- They also resist flexion shear forces. They can generate up to 60N force per muscle. Sometimes 80-100 N force is needed, so the multifidus is overpowered.
Normal Lumbo Pelvic Rhythm
With normal bending the sine flexes first from 60° of lordosis to 20° of kyphosis. The pelvis then flexes through the hip joint (limited by hamstrings and capsule).
Normal flexion causes increased shear forces at L4-5 and L5-S1 at about 20° of flexion.
Pelvic Tilting or Rotation
Tight hams cause posterior tilting of pelvis. This flattens the sacrum. This causes less shear through the sacrum.
So someone who has pars interarticularis fracture, the want to reduce their shear force because the natural door stop to the shear i.e. the facet joint is ineffective. So they tighten their hams to rotate the pelvis backwards to reduce the shear force. So they will have hams tightness / contracture.
Diurnal Disc Height Changes
- Pressure on disc when upright reduces height of disc.
- Recumbent position reduces pressure allowing imbibition to fully rehydrate disc thus increasing disc height.
- Less nuclear pressure might allow greater chance of annular stress later in the day i.e. there is a higher chance of annular injury if someone has been standing all day.
- Muscle fatigue increases load on discs at the end of the day.
Disc Height loss with Degeneration
- Pressure drop of nucleus due to cellular disruption reduces interstitial matrix volume.
- Pressure drop increases annular fibre stress and buckles fibres.
- Disc has more pressure in the morning. Later on in the day the pressure reduces.
Rotation Loads on Annulus
- Annular fibres are at 30° alternating in each layer.
- Rotational load reduces disc annular strength by 50%.
- The fibres aligned with the rotational direction are put under tension and the opposite fibres are unloaded.
- So just by rotating one loses 50% of disc strength.
Flexion loads the posterior annular fibres
The PLL can stretch much further than the posterior annulus can.
With bending the front disc fibres slacken and the posterior fibres are put under stretch.
So with bending one loads the posterior fibres, then if one rotates, 50% of fibres are now unloaded and other 50% are under maximum load.
Greatest stress on posterior annulus occurs with BLT (Bend, Load, Twist).
Positional Changes effect on Intradiscal pressures
A swiss researcher measured disc pressure by putting a needle into the disc.
- Supine: 25
- Sidelying: 75
- Standing: 100
- Standing + bending forwards: 150
- Standing + bending forwards + weight: 220
- Sitting in a chair: 140
- Sitting + bending: 185
- Sitting + bending + load: 275
Mechanical Stress with Flexion on Lumbar discs
- Flexion loads the anterior coloumn (discs) thus increases shear forces.
- Distance from fulcrum (sacrum), spine load increases logarithmically.
- Opposition to flexion stress is provided by erector spinae and multifidus (but is overpowered by load).
- Passive restraints are interspinous ligaments, PLL and posterior annulus. So keep the load close to the body.
BLT
- Flexion causes all posterior annulus fibres to be under tension.
- Rotation causes 50% annulus fibres to off load.
- Remaining fibres load under tension.
- Loading the spine – especially with a weight further away from the body can cause annular tear.
- Genetics play a role here. Some people have good collagen fibres and they don’t tear with these loading activities.
Annular Tears
- The annulus is highly innervated with nociceptors.
- The nucleus is full of inflammatory factors (metaloproteases, arachidonic acid, cytokines).
- Tears allow nociceptors to come into contact with these factors which get activated.
Q: Why sometimes it takes a little while before it becomes painful. That is they wake up the next day with pain.
It is so because of the arachidonic cascade. It takes a while for arachidonic acid to go down the leukotriene, cytokine pathway.
Centre of Rotation
- Normally it is posterior 1/3 of the disc in extension and anterior disc in flexion.
- With degeneration, the COR changes dramatically. (Rolander’s study from 1970s)
Spinal Changes with Flexion / Extension
- Spinal canal is in post 1/3 of spine.
- With flexion COR is in the front, the foramen opens up, the spinal canal opens. There is pressure on the annulus, the facets are distracted.
- With extension, the front annulus is under tension (stretched), the posterior annulus is compressed. The foramen gets narrowed, the spinal canal gets narrowed. The facets overlap more (imbricated).
- Therefore extension causes narrowing of the spinal canal, lateral recess and foramen.
- So with extension, the root will be further compressed. So someone who gets leg pain with extension is getting foraminal or lateral recess stenosis or even central stenosis.
- With forward flexion, if the disc degeneration is advanced there can be bony abutment anteriorly which will cause back pain due to disc pain.
Central Stenosis
- Narrowing of central canal.
- Disc bulge + bone spurs – common cause
- Ligamentum flavum stretches with flexion and comes out of the canal. With extension it bunches into the canal and creates compression.
- This is why people with central stenosis are not good when standing straight. They want to sit or bend forwards or lean on a counter to reduce pressure on the nerves.
- This is dynamic compression. So in this case you see no neurological findings on exam. It doesn’t have enough time to cause an injury to the nerve root.
Basic Rules of Flexion
- Flexion compresses the disc and off loads the facets and pars defects.
- Flexion places posterior annulus under tension. So in annular tear pain increases in flexion.
- Flexion opens the canal, both central canal, lateral recess and foramen.
- Flexion increases shear forces to the lower vertebra (spondylolisthesis)
- Flexion stretches the sciatic nerve (L4-S1) and relaxes the femoral nerve (L2-4).
- Herniated disc symptoms are increased for L4-S1.
Basic Rules of Extension
- Extension narrows the central canal, foramen. So stenosis is made worse by extension.
- Extension reduces pressure on the disc but compresses facets. Patients with bad disc pain want to bend backwards all day long but with bad facets, they are painful.
- Extension relaxes the sciatic nerve but tensions the femoral nerve.
- Extension loads pars fractures (before developing foraminal stenosis)
- Extension reduces shear forces
- Lateral bending with extension compresses the ipsilateral foramen and opens the contralateral foramen.
- HNP L4-S1 patients like extension (offloads sciatic nerve)
- Extension and ipsilateral bending ** Spinal Phalen **
Pelvic Tilt and Lumbar Lordosis
Anterior pelvic tilt increases lordosis, decreases discal pressure and increases facet pressure. This helps patients with degenerative disc disease. In sitting, a lumbar roll helps because it causes extension.
Posterior tilt reduces lordosis, increases disc pressure and decreases facet loading. Patients with bad facets like to flatten their lumbar spine. Patients with stenosis like to flatten the spine.
Facets
Articular cartilage is 70% better. it is responsible for cushioning bone from impacts.
When disc degenerates, increasing pressure and aberrant motion causes cartilage fibrillation. It causes spur formation and causes foraminal or lateral recess stenosis. Cartilage erosion causes the facets to become incompetent which allows a slip which is step 1 in a degenerative spondylolisthesis.
Enthesopathy
- Sharpey’s fibres connect annulus to bone.
- When these partially avulse by aberrant motion, periosteum is pulled off.
- New bone formation occurs at junction of bone and sharpey’s fibres (osteophyte formation).
- Classic example is annulus bulge pulling off PLL or ALL with subsequent spur formation.
- This is the most common cause of cervical radiculopathy and lumbar foraminal stenosis (along with disc height loss).
Flat Back Syndrome
- Lumbar lordosis positions head and torso over the pelvis.
- Loss of lordosis causes head forward over the torso.
- To balance this, the knees flex to posteriorly rotate pelvis to reduce sacral angle.
- This requires a lot of energy from quads and gluteus contraction.
- Straightening the knees causes a forward torso.
Causes of Flat Back Syndrome
- Antalgia – secondary to central stenosis, lateral recess stenosis and foraminal stenosis.
- Lumbar DDD with loss of lordosis (discs produce lordosis, degeneration reduces it)
- Facet pain / spondylolisthesis (rare)
- Thoracic hyperkyhosis wtih poor lumbar compensatory mechanism (bent knees to compensate)
- Hip / Knee flexion contractures
- Hams and gluteal weakness (L5 and S1)
Flat Back due to Stenosis
- Spinal canal widens with flexion and narrows with extension.
- Stenosis will cause flat back positioning to prevent constriction of cauda equina.
- Extension will cause leg / buttock symptoms.
- Removal of stenosis will allow patient to resume normal posture. Also true in lateral recess and foraminal stenosis.
- This is antalgia, not a structural disorder.
Scoliosis Vs Antalgic Rotation
- Spinous process is equidistant from facets (owl eyes) on X-ray in AP view.
- With scoliosis, there is vertebral rotation associated with the curve.
- With antalgic list, there is no vertebral rotation with the curve. (although there is a lateral curve but there is no rotation, so the facets remain equidistant from spinous processes.)